The Role of Technology in Transforming Diabetes Clinical Trials
Diabetes affects millions of people worldwide with blood conditions that change the way they live their day-to-day lives. So, scientists and doctors alike are constantly looking for ways to improve treatment options and enhance patient outcomes. Clinical trials are one of the main ways to gather information from those who actually suffer from diabetes. As well as having allowed us to grow our overall knowledge of the disease. These trials allow us to test new treatment methods and bring them into the market as well. Over the past couple of decades, the growth of technology has transformed diabetic clinical trials to streamline data collection. Additionally, it has improved the patient experience overall. Continue reading to discover the various ways tech has revolutionized the diabetic clinical trial space.
-
User-Based Tech and Remote Monitoring
Technological advances that created the rise of smartwatches also saw the rise of wearable tech that patients can wear full-time. This full time use allows doctors to continuously track data from the patients that are participating in clinical trials, and adjust those trials in real time to adapt the information.
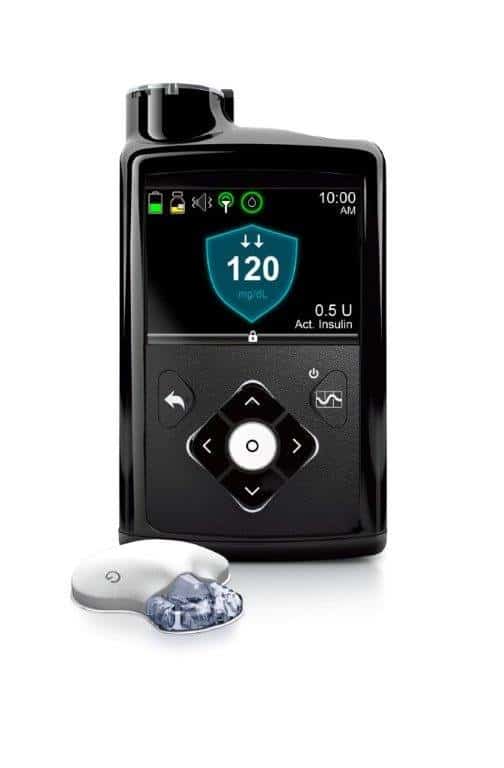
Similarly, the development of user-based technology like fully automatic insulin pumps, continuous glucose monitors (GCMs). As well as other equipment gives patients full-time treatment without ever needing to visit the doctor’s office. User-based tech benefits researchers as well, because they can see how the patients are responding to treatment. Technology takes out human error, so researchers can constantly track the progress of their patients without having any doubt about the data.
-
Big Data and Crowd-Sourcing
The vast database across the Internet, combined with the new methods of monitoring mentioned in the previous section allows researchers to access massive amounts of information when they need to. This information informs doctors and researchers alike about the safety and effectiveness of various treatments or methods of patient evaluation. Scientists are also able to see the long-term outcomes of these methods. This also helps influence their decision-making in a positive way for the patients.
Software has been built specifically for global collaboration, making the work of the doctors themselves much easier. These clinical research management tools create an all-in-one platform for patient and doctor relationships and vastly increase the ease at which information is gathered and distributed.
-
Artificial Intelligence
As our ability to access data worldwide has grown, so has our ability to sort and analyze it with artificial intelligence. AI discovers patterns in data that we might otherwise not, and attribute these patterns to things that we may not even be aware of. Algorithms can provide solutions to problems that are far more complex than the data itself might suggest.
Artificial intelligence can also identify certain patients that are applicable for trials and experiments, depending on what symptoms they show. So, clinical trials are much more streamlined under the watchful eye of AI. Machine learning algorithms also predict patient responses to various treatments and create personalized health plans for them, which of course improves the success rate of the trials.
-
Virtual Appointments
The biggest advancement in clinical research may be telemedicine. It allows researchers to assess patient status, monitor treatments, and communicate virtually, all without ever leaving their office. Because of this, a doctor can now meet with a patient on the other side of the world. While, never having to worry about any of the geographical barriers that would otherwise have stopped them from meeting entirely. Virtual appointments have allowed for the mass diversification of the patient pool, and also give patients in under-privileged areas opportunities that they may not have had otherwise. The appointments also keep the patients themselves accountable, as they receive consistent check ins from the doctors, boosting overall engagement in the clinical trials.
-
Patient Engagement and Health
Despite all of the technological advancements made in the diabetic clinical health world, these trials could not be completed without the patients themselves. The trials are oftentimes very grueling both mentally and physically. Furthermore, the patients have to be intrinsically motivated in order to complete them. For example, hormone levels were tested in children with specific heights and weights. The role of technology in transforming diabetic clinical trials, these children had to adhere to the requirements of the trial. Regardless of the difficulty level of each individual trial, technology has allowed researchers to make the tests as easy as possible on the patients.
Technological advancements also empower the patients, as they feel they can actually be a part of the experiment. And not just participate in it. This feeling of ownership greatly increases the overall quality of the clinical trials themselves. As a result, the patients not only want what is best for themselves but what’s is best for the trial. So, they participate and engage more in the guidelines of the trial. The patient-to-patient aspect of clinical trials is also improved, as they can now communicate regardless of where they are located around the world. Hopefully this article opened your eyes to the role of technology in transforming diabetic clinical trials today.