Understanding The Differences Between Type 1 and Type 2 Diabetes
Diabetes in any form is a condition involving the inability of the body to efficiently carry glucose to the body’s cells and convert it into energy. The key to this issue has to do with the amount of insulin the pancreas produces. However, without sufficient insulin, glucose collects in the bloodstream and is capable of triggering a wide range of diabetes-related health issues. Discussions about diabetes are likely to focus on two types: type 1 and type 2. What sets them apart? And, understanding the differences between t1d and t2d.
Here are four areas where knowing which form of diabetes is present matters.
Diabetes and Insulin Production
The ability for the pancreas to manufacture insulin is often cited as the chief difference between type 1 and type 2 diabetes. However, when no insulin is produced naturally, type 1 is present. The only way to deal with high levels of blood glucose is to introduce insulin from an outside source.
Persons with type 2 diabetes still produce some amount of insulin; it’s just not at a normal level. That means there must be some way to make the most of the insulin that the body does produce. Typically, this involves limiting the amount of simple or complex carbohydrates that are consumed, while using physical activity to stimulate the usage of glucose in the body. Oral medication is also used to help remove excess glucose from the bloodstream.
Forms of Treatment
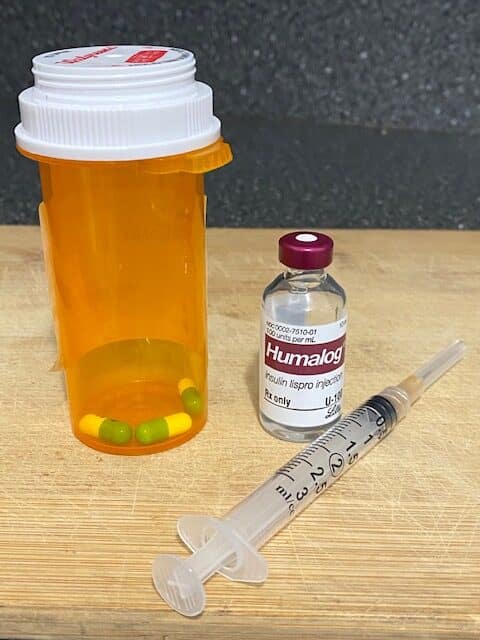
For type 1 diabetics, insulin injections or the use of insulin pumps are the most effective modes of treatment. Over the years, attempts to produce some type of oral medication for type 1 diabetics has met with no success. One of the chief obstacles is that it’s not possible to take insulin orally and have it get into the bloodstream. Enzymes in the stomach break down the insulin before it can be absorbed into the blood. At present, only direct introduction into the cells by means of injections or pumps produce the desired result.
Type 2 diabetics do have access to a wider range of medications. Oral medications are usually considered the first line of defense. If one is not enough to aid in maintaining healthy glucose levels, it’s possible to take two or more. Some help slow the introduction of glucose in the blood while others focus on moving glucose out of the blood and into the kidneys. The latter makes it possible to eliminate excess glucose through urination.
It’s also possible for type 2 diabetics to augment oral medications with injections. This treatment includes the use of insulin in more advanced cases. For a type 2 diabetic, it may be possible to utilize insulin injections in conjunction with an oral medication.
Potential for Low Blood Sugar
Both type 1 and type 2 diabetics can experience low blood sugar as well as high blood sugar. Typically this is more of a concern with those living with type 1. When insulin is taken and the individual does not consume a reasonable amount of carbohydrates, blood glucose levels can drop to an unsafe level. This may result in confusion, fainting, and other consequences. Quickly ingesting some form of carbohydrate will correct the imbalance.
While this is less likely to happen to someone with type 2 diabetes, it’s not unheard of. Checking glucose levels at the one and two-hour marks after eating can reduce the risk. If the level is slightly low, ingesting a small amount of a complex carbohydrate is usually sufficient.
Conclusion
Keep in mind that diabetics of all types should utilize diet, exercise, and proper doses of medication in order to manage their conditions. If you have noticed that your glucose levels are not controlled, work with your doctor and a dietitian to adjust the treatment plan. You’ll feel better, reduce the risk of complications, and in general enjoy a higher quality of health.
Learn about a type of diabetes that is commonly found in youngsters called MODY.