Dawn Phenomenon: Symptoms, Causes and Treatment
The Dawn Phenomenon is a natural yet problematic condition that affects millions of people with diabetes worldwide. This comprehensive guide will help you understand what it is, its symptoms, causes, diagnostic methods, and treatment options to better manage this common diabetes-related challenge.
What is Dawn Phenomenon?
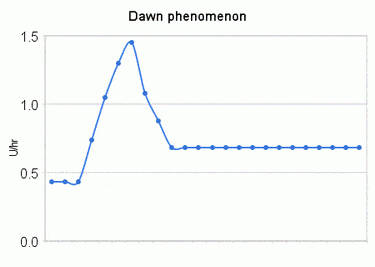
The Dawn Phenomenon refers to periodic episodes of hyperglycemia (high blood sugar) that occur in the early morning hours, typically between 3:00 AM and 8:00 AM, in people with diabetes. This condition is characterized by a spontaneous rise in blood glucose levels that happens naturally as the body prepares to wake up, but becomes problematic in individuals with diabetes who cannot adequately regulate their blood sugar levels (Cleveland Clinic) (ADA).
Unlike the Somogyi effect, which is caused by rebound hyperglycemia following overnight hypoglycemia, the Dawn Phenomenon occurs without any preceding low blood sugar episodes. It affects approximately 50% of people with both Type 1 and Type 2 diabetes across all age groups, making it one of the most common complications in diabetes management StatPearls.
Recognizing the Symptoms of Dawn Phenomenon
The Dawn Phenomenon typically presents with symptoms similar to general hyperglycemia. Key symptoms to watch for include:
Primary Symptoms
- Consistently elevated morning blood glucose readings (often 20 mg/dL or higher than bedtime levels)
- Worsening A1C levels over time
- Difficulty achieving morning blood sugar targets despite proper bedtime control
Associated Hyperglycemic Symptoms
- Increased thirst (polydipsia)
- Frequent urination (polyuria)
- Fatigue and weakness upon waking
- Nausea or upset stomach in the morning
- Blurred vision
- Headaches
It’s important to note that the Dawn Phenomenon is not associated with nocturnal hypoglycemic episodes, which helps distinguish it from the Somogyi effect American Diabetes Association.
Understanding the Causes of Dawn Phenomenon
The Dawn Phenomenon results from complex hormonal interactions that occur naturally during the early morning hours. Understanding these underlying mechanisms is crucial for effective management.
Hormonal Triggers
The primary cause involves the release of several key hormones between 3:00 AM and 8:00 AM:
1. Cortisol (Stress Hormone)
- Peaks in early morning hours
- Stimulates glucose production in the liver
- Increases insulin resistance
2. Growth Hormone
- Naturally surges during sleep
- Promotes glucose release from liver stores
- Has insulin-antagonistic effects
3. Epinephrine and Norepinephrine
- Released as part of the body’s natural awakening process
- Stimulate glucose production
- Prepare the body for daily activities
The Role of Insulin Deficiency
In people without diabetes, the pancreas responds to these hormonal changes by releasing additional insulin to maintain normal blood glucose levels. However, individuals with diabetes face two main challenges:
For Type 1 Diabetes:
- Complete inability to produce insulin naturally
- Dependence on external insulin that may not provide adequate coverage during dawn hours
- Potential waning of long-acting insulin effectiveness
For Type 2 Diabetes:
- Insufficient insulin production to counter morning hormone surge
- Increased insulin resistance during early morning hours
- Impaired ability to suppress hepatic glucose production Mayo Clinic
Contributing Factors
Several additional factors can influence the severity of Dawn Phenomenon:
- Sleep patterns and quality
- Stress levels and cortisol fluctuations
- Timing and dosage of diabetes medications
- Evening meal composition and timing
- Physical activity levels
- Overall diabetes control
Diagnostic Tests for Dawn Phenomenon
Accurate diagnosis of Dawn Phenomenon requires careful monitoring and specific testing approaches to distinguish it from other causes of morning hyperglycemia.
Continuous Glucose Monitoring (CGM)
The gold standard for diagnosing Dawn Phenomenon is continuous glucose monitoring, which provides comprehensive 24-hour glucose data Cleveland Clinic.
Benefits of CGM for Dawn Phenomenon Diagnosis:
- 24/7 monitoring without sleep disruption
- Detailed overnight glucose patterns
- Elimination of Somogyi effect (rules out nocturnal hypoglycemia)
- Quantification of glucose rise magnitude
- Documentation of timing of glucose elevation
Traditional Blood Glucose Monitoring
For patients without access to CGM, healthcare providers may recommend:
Strategic Timing Protocol:
- Bedtime glucose check (around 10:00 PM)
- Middle-of-the-night check (2:00-3:00 AM)
- Morning fasting glucose (upon waking)
Interpretation Guidelines:
- Dawn Phenomenon suspected: Normal bedtime glucose, normal 2-3 AM glucose, elevated morning glucose
- Somogyi Effect suspected: Normal bedtime glucose, low 2-3 AM glucose, elevated morning glucose
- Insufficient insulin coverage: High bedtime glucose continuing through the night
Quantification Methods
Researchers have developed specific formulas to quantify Dawn Phenomenon magnitude:
Standard Calculation: Dawn Phenomenon Magnitude = Morning Glucose – Overnight Glucose Nadir
Alternative Formula (Monnier et al.): For patients unable to use CGM, the magnitude can be estimated using: 0.49X + 15, where X = Pre-breakfast glucose – Average of (Pre-lunch + Pre-dinner glucose)
A glucose rise of 20 mg/dL or greater is generally considered clinically significant StatPearls.
Comprehensive Treatment Options
Managing Dawn Phenomenon requires a multifaceted approach that may include medication adjustments, lifestyle modifications, and advanced diabetes management technologies.
Insulin-Based Treatments
Insulin Pump Therapy (Most Effective)
- Programmable basal rates to increase insulin delivery during dawn hours
- Precise timing control to match hormonal surges
- Flexibility to adjust based on individual patterns
- Superior glycemic control compared to long-acting insulin injections
Long-Acting Insulin Adjustments
- Timing modifications: Moving injection from morning to bedtime
- Dose adjustments: Carefully calibrated to avoid nocturnal hypoglycemia
- Ultra-long-acting insulin: Consider insulin degludec for extended coverage
- Twice-daily basal insulin: Split dosing for better coverage
Rapid-Acting Insulin Strategies
- Small correction doses upon waking (with medical supervision)
- Pre-breakfast insulin timing adjustments
- Insulin-to-carbohydrate ratio modifications for morning meals
Oral Medication Options
While oral medications are generally less effective than insulin for Dawn Phenomenon, some options may help:
- Reduces hepatic glucose production
- Improves insulin sensitivity
- May help with mild Dawn Phenomenon
- Best taken at bedtime for morning effect
Other Considerations
- Acarbose: May provide some benefit in recent studies
- Sulfonylureas: Generally ineffective for Dawn Phenomenon
- SGLT-2 inhibitors: Limited evidence but may help with overall glucose control
Lifestyle Management Strategies
Evening Nutrition Modifications
- Avoid late-evening carbohydrates (3 hours before bedtime)
- Increase protein-to-carbohydrate ratio at dinner
- Consider light, protein-rich bedtime snacks for some patients
- Maintain consistent meal timing
Exercise Interventions
- After-dinner walks: Help reduce overnight glucose levels
- Morning exercise: Can help burn excess glucose from Dawn Phenomenon
- Caution with late-evening exercise: May cause delayed hypoglycemia
- Consistency is key: Regular activity patterns help stabilize glucose
Sleep and Stress Management
- Consistent sleep schedule to regulate hormonal patterns
- Stress reduction techniques: Meditation, yoga, or counseling
- Adequate sleep duration (7-9 hours for adults)
- Sleep quality improvements: Address sleep apnea or other disorders
Preventing Dawn Phenomenon Complications
While Dawn Phenomenon cannot always be completely prevented, several strategies can minimize its impact and prevent complications.
Early Detection and Intervention
Regular Monitoring
- Consistent glucose tracking to identify patterns
- Quarterly A1C testing to assess overall control (Try our A1C Calculator to estimate your average glucose levels over the past 2–3 months.)
- Annual comprehensive diabetes reviews
- Prompt reporting of morning highs to healthcare providers
Proactive Management
- Address Dawn Phenomenon early in diabetes progression
- Prevent insulin resistance worsening through lifestyle measures
- Maintain optimal weight to improve insulin sensitivity
- Regular medication reviews and adjustments
Long-Term Health Protection
Cardiovascular Risk Reduction Research shows that every 1% reduction in A1C can decrease cardiovascular complications by 15-20%. Since Dawn Phenomenon can contribute up to 0.4% to overall A1C levels, managing it effectively provides significant health benefits StatPearls.
Comprehensive Care Approach
- Blood pressure management
- Cholesterol monitoring and control
- Regular eye and kidney function screening
- Foot care and circulation assessment
Frequently Asked Questions About Dawn Phenomenon
Conclusion
Dawn Phenomenon is a common but manageable aspect of diabetes care that affects millions of people worldwide. Understanding its causes, recognizing its symptoms, and implementing appropriate treatment strategies can significantly improve your diabetes management and overall health outcomes.
The key to successfully managing Dawn Phenomenon lies in accurate diagnosis through continuous glucose monitoring, individualized treatment approaches that may include insulin adjustments, medication timing changes, and lifestyle modifications, and consistent collaboration with your healthcare team.
Remember that there’s no one-size-fits-all solution for Dawn Phenomenon. What works for one person may not work for another, and it may take time to find the optimal management strategy for your specific situation. The most important step is recognizing the pattern and working proactively with your healthcare provider to address it.
With proper management, most people with Dawn Phenomenon can achieve their glycemic targets while avoiding the complications associated with persistent morning hyperglycemia. Stay committed to monitoring your patterns, following your treatment plan, and maintaining open communication with your diabetes care team for the best possible outcomes.
Want to learn more about diabetes conditions and complications? Check our articles on polyphagia (excessive hunger), hyperphagia (pathologic hunger), reactive hypoglycemia and LADA diabetes.
There are many different ways to counter this condition which will help, but you should definitely discuss this with your doctor first! Checking your blood sugar first thing in the morning always helps!
Since I’m using an insulin pump, I just program it to release less insulin between midnight and 3am then program more insulin from 3am to 8am. At 8:00am I go back to my normal basal rate for the day. Remember to always consult with your healthcare provider first for personalized diabetes management recommendations. Hopefully you find this info helpful.