How to Manage Diabetes with Exercise and Control your Blood Sugar
Diabetes is currently the leading cause of death in the US and experts estimated that over 500 million people would be affected by type 2 diabetes by 2030. § T2D usually developed through a sedentary lifestyle over time, not a genetic disorder. We all know that exercise helps us live longer. However, a recent study goes one step farther by discovering that a sedentary lifestyle is much worse than smoking, obesity, diabetes and cardiovascular disease. §
According to this research, the risk associated with death is 500% higher in people who have a sedentary lifestyle compared to top exercise performers. This rate is three times higher than smoking. This study was not based on patients self-reports but objectively testing their activities for accurate measurement. Cardiovascular disease and diabetes have been the most costly diseases in the USA, according to Dr. Jordan Metzl. He says “Instead of paying over $200 billion annually for treating these types of diseases and their complications; we need to encourage our communities to become more active and exercise every day”. § So we want to shed some light on how to manage diabetes with exercise.
The Importance of Exercise for Diabetes Control: both types
Exercise makes it a lot easier to control your blood sugar level and benefits individuals with both kinds of diabetes since it raises insulin sensitivity. That means after the workout, your body does not require as much insulin to process carbohydrates.
Individuals with type 1 diabetes (T1D) can acquire the very same benefits from exercise as anybody else. But, studies reveal that lots of people with T1D don’t take part in routine physical activity because of a fear of hypoglycemia or dangerously low blood sugar levels.

Athletes and scientists with T1D both state that patients with diabetes type 1 can exercise safely and efficiently. You can do it by observing the way your body reacts to exercise, learning how to balance food, insulin, and physical activity, and utilizing research-supported strategies to lessen the possibility of hypoglycemia.
Exercise is as essential as diet and medicine for diabetics, and the American Diabetes Association suggests at least 30 minutes of workout that raises the heart rate five times per week to gradually manage diabetes with exercise.
How to Manage Diabetes with Exercise and Get Results
Muscle contraction during workout increases sugar uptake as insulin does, and it’s so effective that a regular exercise program can potentially reduce the risk of type 2 diabetes by 58%.
Exercise may also help individuals with type 1diabetes by preventing long-term complications, particularly heart problems as they are more vulnerable to arteriosclerosis, which may result in a heart attack.
Additionally, developing T2D can cause many other health complications and increases the risk of premature death since it’s strongly connected with cardiovascular disease, the leading cause of death worldwide.

If you stick with a regular fitness program, you can finally manage diabetes with exercise and get these results:
- Improved insulin sensitivity
- Reducing blood glucose levels
- Heightened energy and endurance during the day
- Weight loss with enhanced muscle mass
- A healthier heart with lower blood pressure
- Sound sleep in the night
- Improved cholesterol, heart rate, and blood pressure levels
- Reduced risk of osteoporosis with stronger bones
- Improved immune system
- Lower stress, anxiety, and depression
What Type of Exercise is Good for Diabetics?
The American Diabetes Association suggests two kinds of exercise for handling diabetes: aerobic and strength training.
Aerobic Exercise
This exercise is done by using your arms or legs at a rhythmic, continuous movement to boost your heart rate. Examples include running, biking, dancing, walking and swimming. Make sure you pick an aerobic exercise that you enjoy and set realistic goals.

Strength Training
Strength or resistance training makes your body more sensitive to insulin and may lower blood glucose.
Association suggests performing strength training exercises at least two times each week, but not two days in a row. Examples of strength training include utilizing weight machines, free weights, and resistance bands, and performing bodyweight exercises like push-ups and sit-ups. Lifting or carrying items around such as water bottles works, too.

Both kinds of exercise may produce hypoglycemia (severe low Blood sugar) in late recovery, frequently when patients are still sleeping. Thus, knowing the physiology of different kinds of exercise and the changes that can affect glycemia during a workout should ensure secure and effective glycemic control plans.
How to Start Exercising to Manage your Blood Sugar
Even minor changes can make a big difference, so take action today and start with something you enjoy so you can stick with it. Beneficial exercise can be as simple as walking every day with your dog or anything that forces you to move your body.
Be sure to speak with your doctor before starting a new Training program. Set modest goals because you are more likely to follow them when they’re realistic.
Individuals with diabetes are at increased risk of heart and vascular diseases and also foot problems; therefore, it’s important to choose an ideal exercise for you.
T1D diabetics may have to start preparing an hour or 2 before starting an activity to ensure that their insulin level is balanced to prevent overeating throughout the workout and simultaneously avoid hitting high blood sugar or hyperglycemia.
Preparations for a workout can be done by adapting short-acting insulin doses, the basal rate on a pump, eating food to counteract the last insulin injection, based on the type of the purposed action and your prior reaction to exercise.
Post-exercise drinks like drinking whole milk can also be a useful tool to avoid immediate hypoglycemia.
Precautions to take before and during exercise
Diabetic patients are at the risk of hypoglycemia, particularly during and after exercise. So be sure you’ve got an individualized diabetes control program tailored by a diabetes specialist.
If you have not been exercising for a long time, start with a less-intense workout, this can help construct exercise tolerance. You’ll also be more inclined to keep on doing routine exercise and avoid injuries.
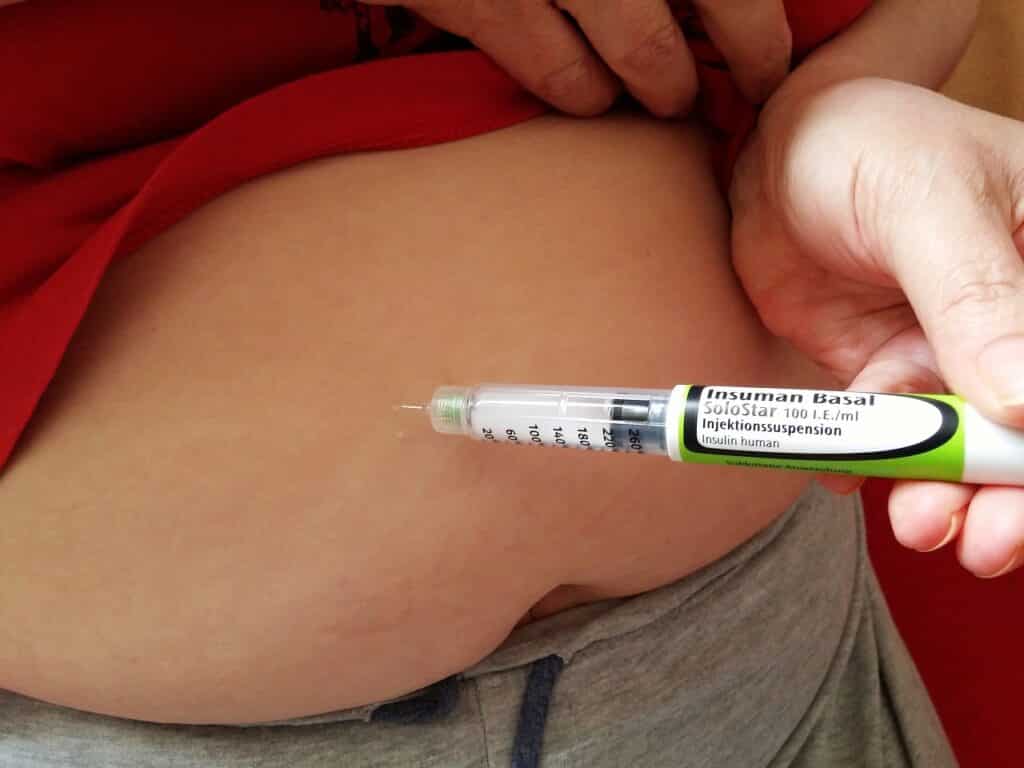
Discuss with your doctor the most suitable parts of your body to inject insulin, particularly during exercise. Also know what’s your blood sugar level is before you start exercising.
Foot Care when Exercising
Individuals who’ve had diabetes for quite a while or those who’ve always substantial BGLs are at higher risk of developing foot issues. In case you have nerve damage for your feet, this makes you more vulnerable to injury and also to problems like foot ulcers. The health of your toes may be assessed by a podiatrist to be sure you’re secure to perform the exercise you’re planning.

Control your Blood Sugar to Prevent Hyperglycaemia
Hyperglycaemia is another condition when BGLs are excessively high, more than 11mmol/L. Diabetic patients who have BGLs over the standard range are more in the risk of dehydration so drink more fluids to stay hydrated once you exercise.
Stay Committed to your Exercise Routine
It’s important to look for a lifelong exercise regimen that’s both attainable and fun. Walking is one of the simplest and most suitable possibilities, but you might choose to explore new alternatives, too! You should exercise at a comfortable rate and don’t overexert yourself.
Some people think committing to a routine exercise program simply requires time management and decision. They can use a diabetes management app such as MySugr, Glucose Buddy, Diabetes: M, and Sugar Sense Diabetes App. Others may benefit from joining a gym to get some motivation.